Competitive shooting is a challenging and enjoyable sport. But, it has a cruel side. It can take years to master the physical and mental skills required to excel. Unfortunately, that point can arrive about the time the inevitable effects of aging begin to interfere with the physical side. Diet and exercise can address some issues, but vision is another matter.
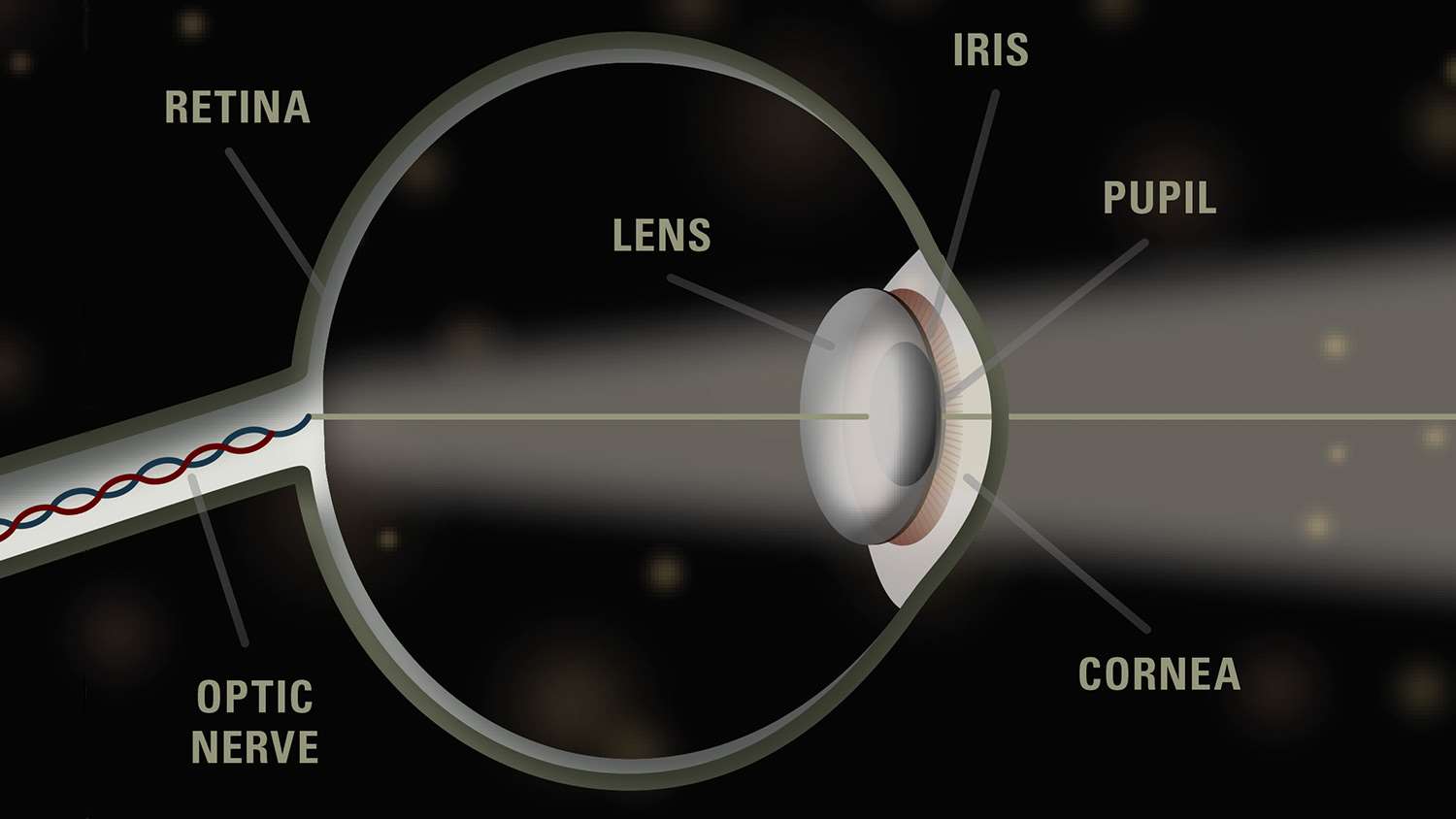
You can’t hit what you can’t see. Vision will deteriorate with age, although corrective lenses can negate some of that. At least, they can until cataracts appear.
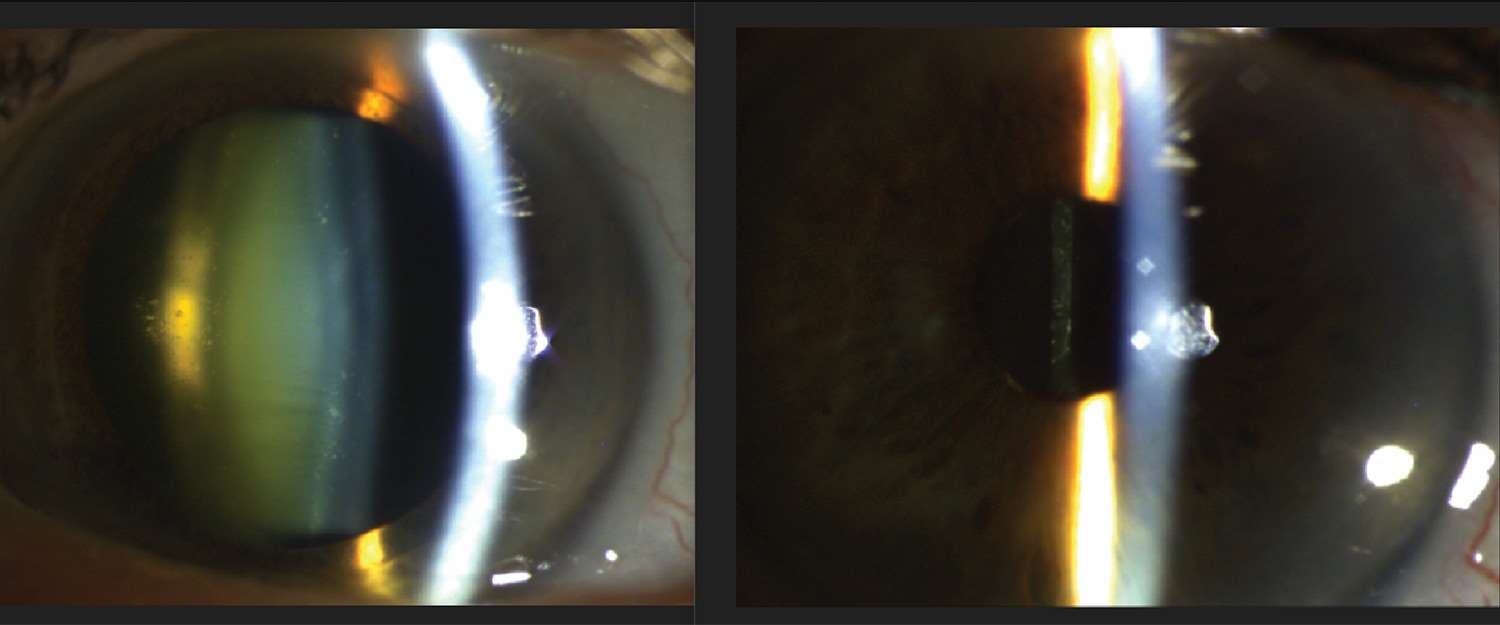
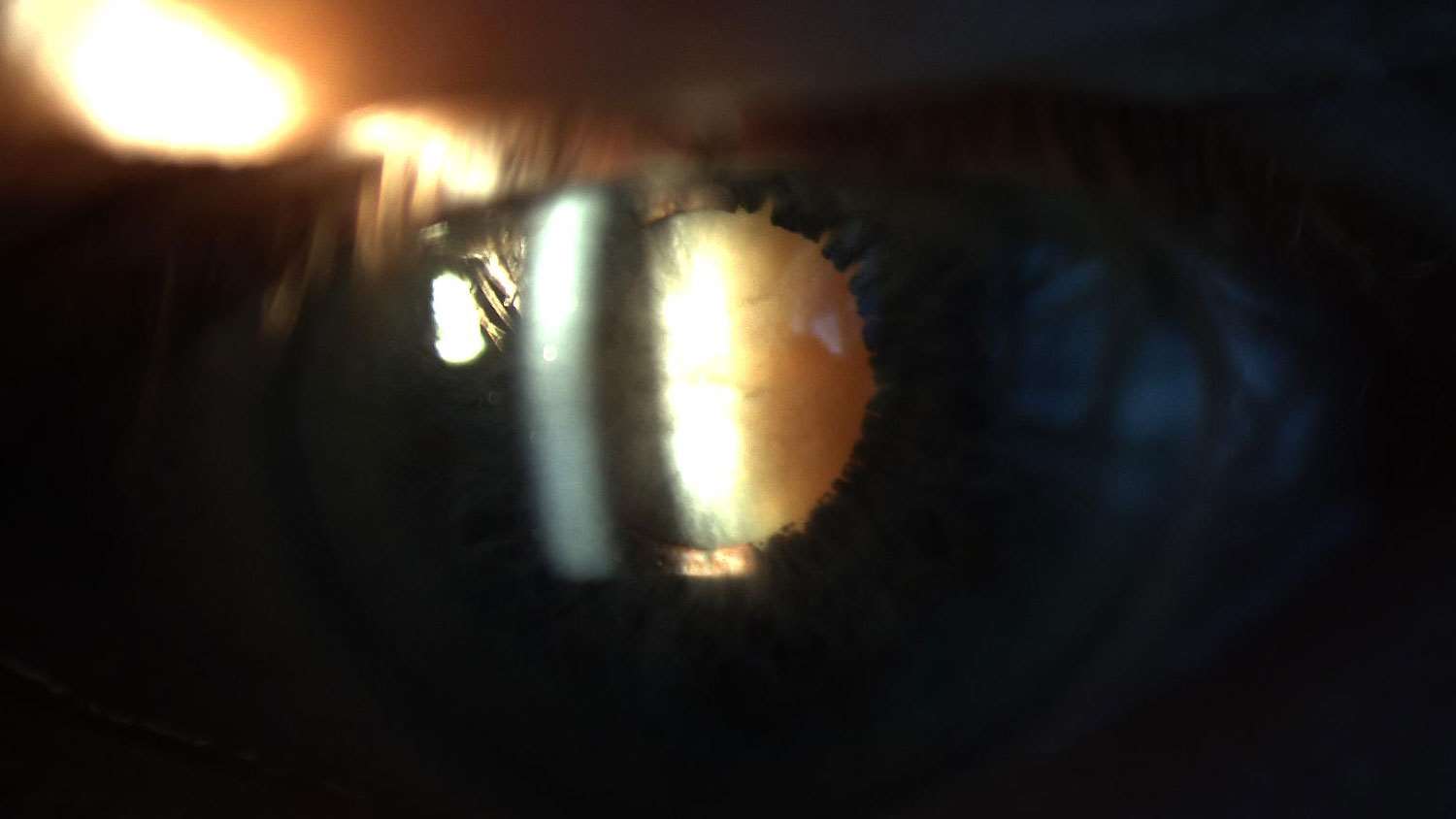
“Cataracts is a term used to describe the opaqueness of the crystalline lens inside the eye,” says Doctor of Optometry, Alexis Rodriguez. “There are many types of cataracts, such as congenital, traumatic, or those caused by medications or secondary to disease. But the most common type of cataracts in the human eye are a group of cataracts that occur during the aging process. As a matter of fact, everyone will eventually get cataracts at some point in their lives.”

“It is difficult to pinpoint the exact age at which we will get cataracts,” he notes. “Our eyes normally begin to age at 40. Although that is young for most patients to have symptoms, it is likely that a doctor can begin to see incipient changes to the crystalline lens that indicates the beginning of cataracts. By age 50 most patients have very mild symptoms and visible mild cataracts can be detected in some patients.”
“The effects upon vision,” Dr. Rodriguez continues, “can depend upon the type of cataract. But the most common complaints are blurry or opaque vision, increased sensitivity to light, and halos around light sources, like automobile headlights at night.”
That is the situation I found myself in when I was diagnosed with cataracts in both eyes about five years ago. Since my teens, my uncorrected vision has been in the “Mr. Magoo range” (well south of 20/200), but corrective lenses kept me close enough to 20/20 to successfully compete on Navy Rifle and Pistol Teams and years later attain Master in IDPA and A Class in multiple Steel Challenge divisions. Unfortunately, the last few years saw my vision deteriorate rapidly as the cataracts in both eyes grew. The best correction for my left eye was now 20/80, and vision was fuzzy. The right eye was a bit better at 20/30, but my vision was adversely-affecting my shooting, and I was relegated to optical sights.
When the effects of cataracts become severe, surgery is a solution. But as with any surgery, there are risks.
“No surgical procedure is simple and without the potential for complications,” Dr. Rodriguez states. “Every patient needs to understand that cataract surgery is an invasive procedure and can have risks. However, it is one of the most common surgical procedures performed in the United States.”
Although the surgery is common, there are limitations.
“The expectation after surgery,” he continues, “should never be that one will not require eyeglasses. Most of the time the patient will have to use distance, or near or bifocals, to fine-tune their vision.”
Dr. Rodriguez also notes that one complication of cataract surgery that may crop in some patients, months or years later, is a condition called Posterior Capsular Opacity. That can produce blurry vision and glare/light sensitivity. But a procedure called the Yag Capsulotomy can correct it.
I had been encouraged by doctors to have cataract surgery. But to say I was apprehensive would be a serious understatement. I was only issued two eyes at birth. They are not replaceable. The thought of someone “digging” into them was frightening. I later learned this was not uncommon among first-time patients. But like many older shooters, I had reached the point where I didn’t have much choice if I wanted to continue competitive shooting at my level.
I made a call to my VA provider at the Gainesville, FL, medical center. I was quickly set up with an optometry appoint for a preliminary eye exam, soon followed by a more comprehensive exam at the Ophthalmology department.
I then met with my VA surgeon, Dr. Wanda Martinez—a petite lady with a warm smile, a keen mind and, as I found out later—a very steady hand. That meeting with the surgeon is important because there is much they can do, once they know what you need or want. They can make you nearsighted, farsighted or craft pretty much what you want your vision to be when they implant the new lenses in the eyes—within limits.
She asked many questions about what I did in my daily life. I explained that I’d been nearsighted all my life, worked on a computer and shot guns. I was very comfortable wearing one set of glasses for computer work and a different set for normal-distance vision, and didn’t want bifocals. She digested all that and came up with a plan. The left eye would be done, and the right eye would be considered later.
I was still very apprehensive about the surgery, but a pre-op nurse knows how to put things in perspective.
“When you have an eye exam,” she said, “they put this big light in your eye. Do you have a problem with that?” I didn’t. She then told me that’s exactly what will happen during the operation, and that I might feel a little gentle pressure on the eye, but there will be no pain. I would be hooked up to an IV with some Valium but would be awake during the operation. “If you can handle an eye exam,” she said, “You can handle this.”
She was right.
A week later I reported for surgery. A friend took on the responsibility of driving me to and from the hospital. That’s standard procedure.

Dr. Martinez, aware of my apprehension, spoke with me before the operation. She was very comforting. The surgery was quick, painless, and my fears about the surgery proved to be groundless.
I left the operating room with a metal and plastic cup taped over my left eye. Two hours later there was a follow-up exam with an intern. The cup was removed, the eye thoroughly checked, and then the cup was handed back to me, along with a roll of tape and instructions to place it back over the eye for the next four nights while sleeping. That would prevent any inadvertent rubbing or other damage to the recent surgery during sleep. Two different eye drops were provided, to be used four times a day for the first four days, with one of the drops to be tapered off. The application of drops continued for several weeks. One was to prevent infection and the other (the continued drops) to prevent inflammation. I would then return in one week for a follow-up exam.
During that week the eye drops were no problem, although the eye cup didn’t help my sleep. I had been told that during the first few days after surgery I might feel a bit of irritation, almost like there was a grain of sand in there, but that it would pass. I had the irritation, and it passed.
My current eyeglasses worked well; both the distance glasses and the closer-focal-point computer glasses that I also used for shooting iron-sight handguns. The new left-eye prescription made the left lens a gray blur, but the right eye was normal. Being strongly right-eye dominant I had no issues functioning with only the right eye. In fact, (although I didn’t tell my doctors this) my surgery was on a Thursday, and by the following Monday I shot an eight-stage Steel Challenge match with my RFRO gun. I even bested two of my classifier times and moved closer to Master.
A few days later was my one-week follow-up exam. The eye was fine, and the left eye test showed 20/20. The intern told me it would be 30 days before they could give me a final prescription. I asked for and received an interim prescription and immediately drove to my local optical shop that offers one-day service. They put a left lens into a spare pair of glasses. I thought life would be good.
I was wrong.
Putting on the new glasses was odd. Closing the right eye, the left eye was perfect. Closing the left eye, the right eye was “normal,” but objects seemed to be a bit smaller than they appeared with just the left eye. With both eyes open there were image jumps and depth perception was poor. I had been told this was a possibility, and that it might take a few days for the “new eye” to start working with the “old eye.” I didn’t feel safe driving with those glasses so I drove home with the old “right-eye” glasses. I spent the next two days around the house with the new glasses to see if the eyes would adjust. They didn’t. A call to the VA had me quickly back with Dr. Martinez. I explained the situation and a week later I was back for right-eye surgery.
Having been through the procedure before there was no fear. It went quickly, and Dr. Martinez and I even chatted during the operation. Then the follow up after two hours, and the eye cup and drops. I was pretty used to that.
The following morning I made the pleasant discovery that the plan Dr. Martinez came up with after our initial consultation was excellent. With both of my “new eyes” working together I no longer needed glasses to work on the computer, or around the house, unless I was watching TV across the room.
I still, as she had told me, would need glasses for outside-distance vision. That created a problem since the “new” right eye made the glasses I had been wearing useless. Both lenses were now gray blurs.
The “left-eye” glasses I had made up after the first surgery were there, and the left eye was perfect. But the blurry right-dominant eye wasn’t happy. I was not comfortable with the vision or depth perception afforded with them and didn’t want to have to go through a week like that. Fortunately, I lucked into a solution.
Like most longtime eyeglass wearers, I had a box full of old prescription glasses. I was looking through those, trying them on to see what frames I might want to have the new prescription lenses put into, when I came across one pair where I could actually see with both eyes. They were over a decade old, before my vision went totally south, and a weaker prescription. They weren’t perfect, but they were functional and I wore those for the week.

The next week’s appointment was a repeat of the first. The eye test was 20/20, wait 30 days for a final prescription, and I got an interim prescription. While I was there I checked the old prescription glasses I had worn that week and they showed 20/40 vision. I guess it pays to save old glasses.
I went back to my next-day service optical shop to have the new right-eye prescription put into the frames holding the new left-eye prescription. When I picked them up and put on, life was good.
Both eyes were sharp and clear. I then had lenses with Extra Active Transition put into another set of frames, since my eyes have always been light sensitive, and cataract surgery will increase that because the new, more transparent, lenses are allowing more light in.
The entire process for both eyes took about four weeks. It wasn’t painful. The only annoyance was wearing the eye cups at night. Although without my finding the “old glasses” the last week might have been a bit rough.
Thirty days later, I was in for my final eye exam. There had been (as I was told there likely would be) a very minor change in the prescription. It was primarily in the left eye. I was still seeing very close to 20/20 (better than 20/25) with the interim prescription. The final prescription just “fine-tuned” things. I also went back to my local optical shop and had a pair made up with that prescription, and a 25-inch focal distance to use with iron sights. My “irons” are now sharp, clear—and so are 35-yard plates. I can even see the hit splashes!
Bottom line? I no longer need glasses to work on a computer and type this. The distance glasses I wear outside have me seeing better than I have in 30 years, and I’m no longer relegated to just optical sights.
I wish I had done this sooner.
Read more vision-related articles: